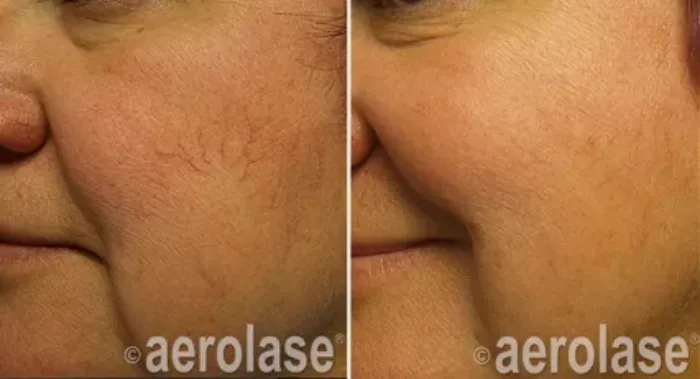
Melasma is a skin condition that causes dark patches, mainly on the face, often seen as the “mask of pregnancy.” It primarily affects women with darker skin tones and can appear symmetrically on areas like the cheeks and forehead. Factors such as hormonal changes, sun exposure, genetics, and stress can trigger melasma. A dermatologist typically diagnoses it through visual examination or specialized tools. Treatment options range from topical solutions to laser therapy. When opting for laser treatment, expect a consultation to assess your condition first. The procedure is generally quick and involves minimal discomfort; however, post-treatment care like sun protection is key for best results.
1. What is Melasma?
Melasma is a skin condition that results in dark, discolored patches on the face, often giving it a mottled appearance. This condition is most commonly seen in women, particularly during pregnancy, which is why it is often referred to as the “mask of pregnancy.” Melasma typically affects those with darker skin tones, but it can appear in anyone. The brownish patches usually manifest symmetrically on areas like the cheeks, forehead, nose, and chin, and they can sometimes extend to the neck and forearms. The patches can be triggered by hormonal changes, such as those occurring during pregnancy or from hormonal medications, and they are worsened by sun exposure, which stimulates the skin to produce more pigment. Other factors that may contribute to melasma include genetic predisposition, stress, and the use of certain medications. Understanding melasma is crucial, as it helps in identifying effective treatment strategies and managing expectations for those seeking solutions.
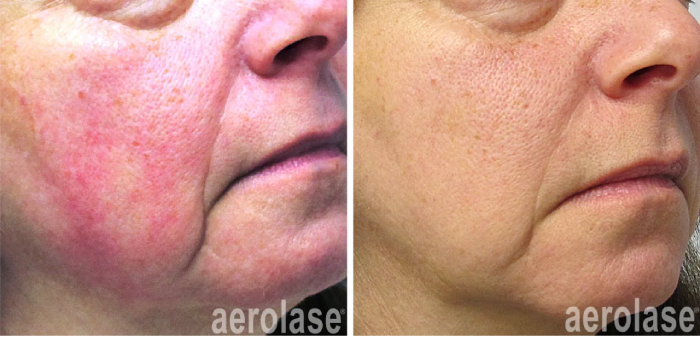
2. Recognizing Melasma Symptoms
Melasma symptoms are primarily characterized by the appearance of brownish patches on the skin, most commonly found on the face. These patches typically develop symmetrically on the cheeks, forehead, bridge of the nose, and chin, giving rise to a distinctive look that many refer to as the “mask of pregnancy.” While the face is the most affected area, melasma can also manifest on other parts of the body, such as the neck and forearms. The discoloration can vary in intensity and may become more pronounced with sun exposure, making it essential to recognize these symptoms early. Individuals may notice that the patches can change in color, becoming darker during certain times, such as hormonal fluctuations during pregnancy or with the use of birth control pills. Furthermore, while melasma predominantly affects women, it can also occur in men, although less frequently. Recognizing these symptoms early can lead to timely intervention and better management of the condition.
3. Causes Behind Melasma
Melasma is a complex skin condition with several contributing factors. One of the primary causes is hormonal changes, which is why it often appears during pregnancy or with the use of birth control pills. These hormonal fluctuations can stimulate the production of melanin, the pigment that gives skin its color, leading to those characteristic dark patches.
Sun exposure plays a significant role as well. Ultraviolet (UV) rays from the sun can trigger an increase in melanin production, exacerbating existing melasma or causing new patches to form. This makes sun protection essential for managing the condition.
Genetics also plays a part; if you have family members with melasma, your chances of developing it increase. Additionally, factors like stress and certain medications, such as those that cause photosensitivity, can contribute to the onset of melasma. For example, some anti-seizure medications may make the skin more reactive to sunlight, leading to pigment changes. Understanding these causes is crucial for both prevention and treatment.
4. How Melasma is Diagnosed
Melasma is primarily diagnosed through a visual examination by a dermatologist. During this examination, the doctor will assess the appearance and location of the discolored patches on your skin. To gain a deeper understanding of the pigmentation, they may use a Wood’s lamp, a specialized tool that illuminates the skin and helps determine the depth of the pigment. In some cases, a skin biopsy may be necessary to rule out other skin conditions that can mimic melasma, such as lentigines or other pigmentary disorders. This thorough approach ensures that the diagnosis is accurate and that the most effective treatment plan can be established.
5. Overview of Treatment Options
There are several treatment options for melasma, each tailored to the severity and specific characteristics of the condition. Topical treatments are often the first line of defense. Hydroquinone is a popular choice, as it helps lighten dark patches when applied regularly. Other topical agents include tretinoin, which speeds up skin cell turnover, and corticosteroids that can reduce inflammation. For more persistent cases, dermatologists may recommend procedures like chemical peels or microdermabrasion, which exfoliate the skin and encourage new cell growth. Laser treatments are particularly effective for stubborn melasma. They work by targeting the pigment directly, breaking it down without harming surrounding skin. Fractional lasers, for example, deliver energy in a controlled manner, allowing for precise treatment. Patients usually require multiple sessions for optimal results, and these can be enhanced with topical treatments. It’s important to consult a dermatologist to determine the best approach based on individual skin type and melasma severity.
- Topical treatments
- Chemical peels
- Microdermabrasion
- Intense Pulsed Light (IPL) therapy
- Laser treatments
- Sunscreen and sun protection strategies
- Lifestyle modifications and home remedies
6. Understanding Laser Treatments
Laser treatments for melasma are designed to target the excess pigment in the skin without causing damage to the surrounding tissue. Different types of lasers can be used, including fractional lasers, which deliver energy in a grid-like pattern, allowing for precise targeting of pigmented areas while promoting healing in the surrounding skin. This method can help break down the melanin deposits that cause the brown patches associated with melasma.
Before undergoing laser treatment, it’s important to have a thorough consultation with a dermatologist to assess your skin type and the severity of your melasma. The effectiveness of laser treatments can vary based on individual factors, such as skin tone and the depth of pigmentation. Typically, a series of sessions is recommended to achieve optimal results, and many patients notice improvements in their skin tone after just a few treatments.
Post-treatment, patients may experience temporary side effects like redness or swelling, but these usually resolve quickly. Effective sun protection is essential after treatment to prevent melasma from returning, as sun exposure can trigger increased pigmentation. Combining laser treatments with topical agents can enhance outcomes, making it a comprehensive approach to managing melasma.
7. What to Expect Before Laser Treatment
Before undergoing laser treatment for melasma, the first step is a thorough consultation with a dermatologist. During this appointment, your doctor will assess your skin type, the severity of your melasma, and your medical history. They may ask about any previous treatments you’ve tried and your expectations from the procedure. This is also an excellent time to discuss any concerns you may have regarding the treatment.
You may be advised to avoid sun exposure and certain medications in the weeks leading up to your treatment. This is crucial because sun exposure can increase pigmentation, making the treatment less effective. Your dermatologist might recommend using a broad-spectrum sunscreen daily to protect your skin.
Additionally, if you are on hormonal medications, such as birth control pills, it’s important to discuss this with your doctor, as these can contribute to melasma. They may suggest adjusting your medication or waiting until after pregnancy if you are planning to conceive.
Expect to receive pre-treatment instructions tailored to your specific situation. These could include guidelines on skin care products to use or avoid, as well as any necessary lifestyle changes to optimize the results of your laser therapy. Being well-prepared can help ensure that you achieve the best possible outcome from your treatment.
8. What Happens During Laser Treatment
During laser treatment for melasma, the procedure begins with the application of a cooling gel or numbing cream to minimize discomfort. The dermatologist will then use a laser device, which emits concentrated light energy targeting the pigment in the skin. The sensation is often likened to a rubber band snapping against the skin, with most patients reporting only mild discomfort. The duration of the treatment typically lasts between 30 minutes to an hour, depending on the size of the area being treated. After the laser session, the skin may appear slightly red or swollen, similar to a mild sunburn. This is a normal response and usually subsides within a few hours to a couple of days. The dermatologist may recommend using specific post-treatment skincare products to soothe the skin and enhance healing. It’s important to follow these recommendations closely to achieve the best results.
9. Post-Treatment Care for Melasma
After undergoing laser treatment for melasma, proper post-treatment care is essential to ensure optimal healing and results. First and foremost, sun protection is crucial. Patients should apply a broad-spectrum sunscreen with an SPF of at least 30 daily, even on cloudy days, and reapply every two hours when outdoors. Wearing wide-brimmed hats and seeking shade during peak sun hours can also help minimize sun exposure.
It’s normal to experience some redness, swelling, or even a temporary darkening of the treated areas following the procedure. Applying a gentle moisturizer can soothe the skin and help with recovery. Avoiding harsh skincare products, such as exfoliants and retinoids, for a few days post-treatment is advisable to prevent irritation.
Additionally, staying hydrated and maintaining a healthy diet can support the skin’s healing process. Patients should avoid strenuous exercise and activities that cause excessive sweating for at least 24-48 hours after treatment, as this can exacerbate irritation.
If any unusual symptoms occur, such as increased pain or prolonged redness, it’s important to contact the dermatologist for guidance. Following these care instructions diligently can help maximize the benefits of the laser treatment and contribute to a more even and vibrant skin tone.
10. Importance of Follow-Up Appointments
Follow-up appointments after melasma laser treatment are crucial for several reasons. Firstly, they allow your dermatologist to monitor the effectiveness of the treatment and make any necessary adjustments. For example, if you notice that certain areas of discoloration aren’t responding as well as others, your doctor can modify your treatment plan accordingly. Additionally, these appointments provide an opportunity to discuss any side effects you may be experiencing, such as redness or swelling, ensuring that your recovery is on track.
Regular check-ins also help in the long-term management of melasma. Since melasma can recur, your dermatologist can provide ongoing advice on maintenance strategies, such as the continued use of topical treatments or lifestyle adjustments to minimize triggers like sun exposure. This proactive approach can significantly enhance the long-term results of your treatment. By attending follow-up appointments, you can take an active role in managing your skin health and achieving the best possible outcomes.
11. Managing Life with Melasma
Living with melasma can be challenging, especially since the condition often affects visible areas of the skin. It’s essential to develop a daily skincare routine that includes gentle cleansing, moisturizing, and broad-spectrum sunscreen to protect against UV rays, which can worsen pigmentation. Many individuals with melasma find that wearing makeup, such as tinted moisturizers or foundations with SPF, helps them feel more confident when going out.
Support groups or online forums can provide a space to share experiences and coping strategies. For instance, connecting with others facing similar challenges can offer emotional support and practical tips on managing melasma. It’s also important to stay informed about the latest treatments and skincare advancements, as new options become available.
Regular check-ins with a dermatologist can help in adjusting treatment plans as needed, ensuring the best possible management of the condition. By incorporating these practices into daily life, individuals can better navigate the ups and downs of living with melasma.
12. Working with Dermatology Professionals
Collaborating with dermatology professionals is crucial for effectively managing melasma. A board-certified dermatologist has the expertise to evaluate your specific skin type and the severity of your melasma. They can recommend personalized treatment plans that may include laser therapy, topical treatments, or a combination of both. During your consultations, it’s vital to discuss your medical history, any medications you are taking, and your skincare routine. This information helps the dermatologist tailor the treatment to your needs. Moreover, dermatology professionals can guide you on post-treatment care and sun protection strategies, which are essential to prevent melasma from returning. They can also monitor your progress, making adjustments to your treatment plan as necessary, ensuring that you achieve the best possible results.
Frequently Asked Questions
1. What is melasma and why is it treated with laser?
Melasma is a skin condition that causes brown or gray patches, usually on the face. Laser treatment helps to reduce these patches by using focused light to break down the excess pigmentation.
2. Is the melasma laser treatment painful?
Most people describe the sensation during the treatment as mild discomfort, similar to a rubber band snapping against the skin. Numbing cream is often used to help minimize any pain.
3. How many laser treatment sessions are usually needed for melasma?
The number of sessions can vary depending on the severity of the melasma. Generally, it may take three to six sessions spaced a few weeks apart for optimal results.
4. What should I expect after a melasma laser treatment?
After treatment, you might notice some redness and swelling in the treated area, similar to a mild sunburn. This usually subsides within a few days, and you can typically resume normal activities.
5. Are there any side effects from melasma laser treatment?
While laser treatments are generally safe, possible side effects include temporary redness, swelling, or changes in skin color. It’s important to discuss any concerns with your dermatologist beforehand.
TL;DR Melasma is a skin condition causing dark patches primarily on the face, especially in women with darker skin tones. Symptoms include symmetrical brownish patches on the face and possibly other areas. Causes involve hormonal changes and sun exposure. Diagnosis involves visual exam and possibly skin biopsies. Treatment options include topical treatments, chemical peels, and laser therapy. Laser treatment is effective but may require multiple sessions, with care needed afterward to prevent sun damage. Ongoing maintenance and follow-up with a dermatologist are essential for managing melasma.
Resource URL: